Deep vein thrombosis: a potential threat to gamers
Key points
Disclaimer
This information is for educational purposes only and is not intended to replace the advice of your doctor. Esports Healthcare disclaims any liability for the decisions you make based on this information.
The information contained on this website does not establish, nor does it imply, doctor-patient relationship. Esports Healthcare does not offer this information for diagnostic purposes. A diagnosis must not be assumed based on the information provided.
IMPORTANT
Deep vein thrombosis is a high risk condition affecting the veins—most often in the lower leg. If you suspect you have deep vein thrombosis, it is important to seek medical care for treatment options. This condition may become more common in gamers due to prolonged periods of time sitting.
What is deep vein thrombosis?
Deep vein thrombosis is clot formation in the deep veins—most commonly in the lower leg. This may occur in gamers due to the lack of movement during long sessions of gaming and/or streaming. The lack of movement can cause the blood flow in the legs to become stagnant, and stagnation triggers the formation of clotting.
If a clot, called a thrombus, forms in the deep veins of the lower leg, the clot could eventually break free. This is a severe health risk. If this occurs, the embolus (free floating clot fragment) will go through the vascular system, through the heart, and eventually may become lodged in the lungs. This condition is known as a pulmonary embolism and is a medical emergency!
Pertinent anatomy
It is important to know some basic anatomy of the vascular system to better understand deep vein thrombosis.
To begin, the word thrombosis is defined as a local coagulation or clotting of the blood in a part of the circulatory system. In deep vein thrombosis, this coagulation or clot formation will occur in the veins deep to your body—as opposed to the veins closer to the surface of your skin, known as superficial veins.
A deep vein thrombosis could happen in the upper or lower extremities (arms or legs), but the risk attributed to prolonged sitting, as seen in gaming, are less likely to affect the upper extremity. Therefore, we will focus on deep vein thrombosis in the lower extremity.
In the legs, the veins most commonly affected are:
- Veins in the thigh (from the hip to the knee)
- Femoral veins: located at the front and upper portion of your thigh
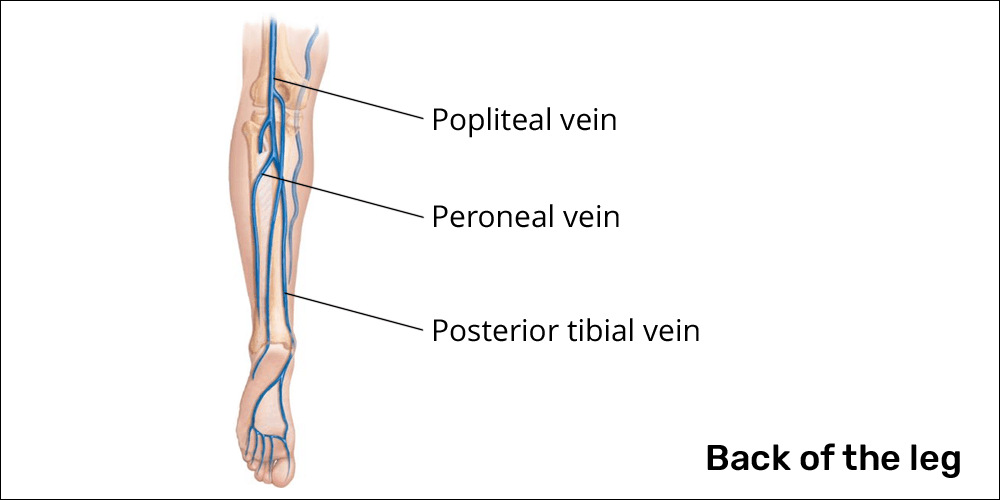
- Popliteal veins: located in the back of your thigh behind the knee joint
- Veins in the leg (from the knee to the ankle)
- Posterior tibial veins: located behind the shin bone within the calf muscles
- Peroneal veins: also located behind the shin bone within the calf muscles but further to the lateral (outer) portion of your leg
Vascular system and pulmonary embolism
From the lowest vein in your foot to your heart, the blood vessels continue to become larger in diameter. Thus, a thrombus breaking off (becoming an embolus) will have no resistance from its break point all the way into the chambers of the heart.
From the heart chambers, the embolus will enter the pulmonary artery—a large vessel from the heart to the lungs. The arterial system from the heart to the lungs rapidly becomes smaller in diameter until it reaches capillaries within the lung tissue.
The embolus may become lodged in these smaller diameter vessels, known as a pulmonary embolism. This is a medical emergency! Common pulmonary embolism symptoms are listed below.
Pathophysiology
Deep vein thrombosis occurs in otherwise healthy individuals when blood flow becomes stagnant or turbulent. Most often, this will occur due to lack of physical activity—as in prolonged sitting during gaming or streaming sessions.
The pumping action of muscles
The veins in your legs—particularly those furthest away from the heart—will not have enough pressure from your beating heart to move the blood upwards against gravity back towards your heart.
Instead, these veins are often positioned between large muscles. When these muscles contract, they become larger in diameter and press on the adjacent veins.
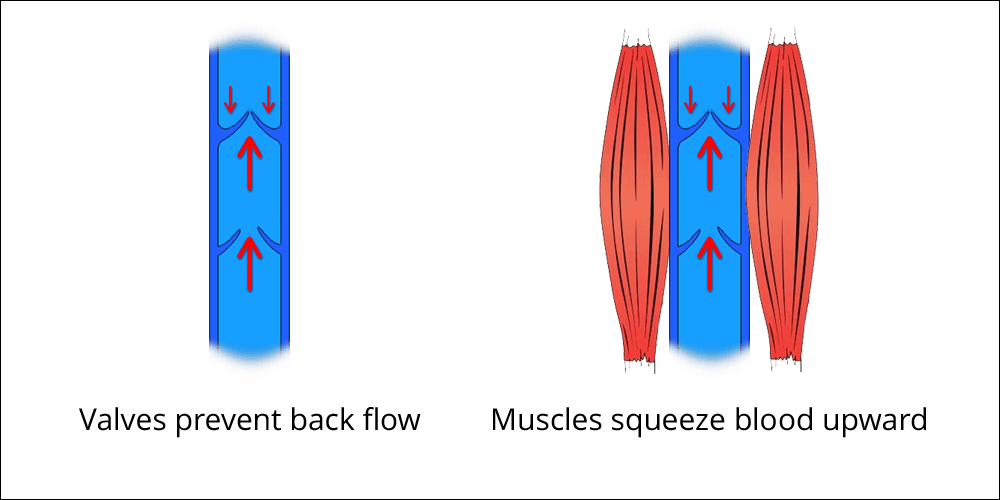
Venous valves
Veins also have a valve system to prevent back flow. These valves have a unidirectional opening back towards the heart, and resistance backwards causes the valves to close. Thus, the valve system along with muscle contraction provides venous blood flow back to the heart.
- Stagnation:
- Stagnant blood flow does not necessarily mean complete lack of flow; rather, stagnation often refers to a decrease in flow velocity
- When blood moves slowly or stops, platelet activation, aggregation, and thrombus formation occur more rapidly
- Turbulence: violent or unsteady movement of fluid
- Turbulence will occur within a blood vessel if there is stenosis (narrowing)—for example, when a thrombus is developing on a vessel wall
- As the blood flow hits the thrombus, the flow is no longer streamlined; picture a creek or small river with a large stone in the center where the water is redirected and flows erratically
- When blood flow is not streamlined, platelet activation, aggregation, and thrombus formation occur more rapidly
Signs and symptoms
If there is a deep vein thrombosis developing in your leg, you may notice the following signs and symptoms. Also note, it is possible, but unlikely, to develop a deep vein thrombosis in both legs at the same time. Most often, these symptoms will present on one side in comparison to the other.
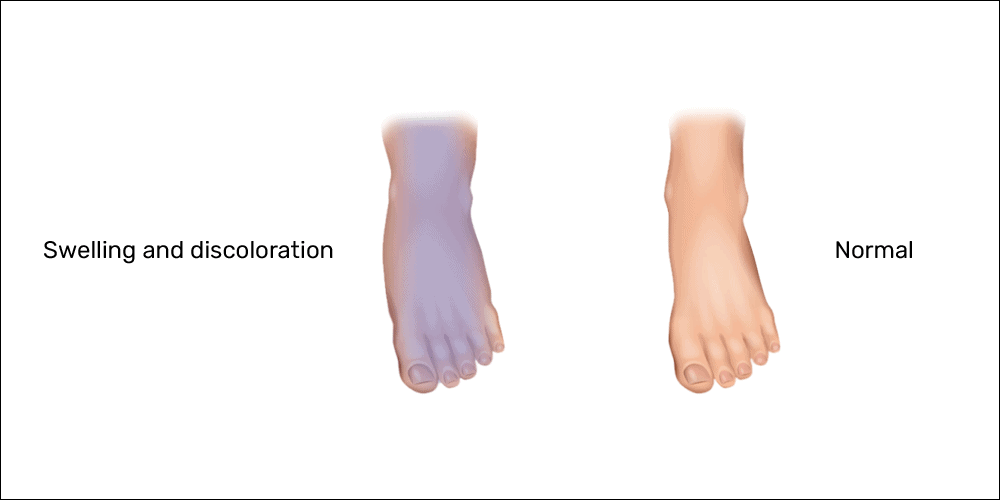
- Swelling
- Swelling in your foot, ankle, or lower leg may develop
- Paleness or blue color to your skin
- Paleness or blue color in your foot, ankle, or lower leg may develop
- Coolness, numbness, or tingling
- Feeling cool or cold, numbness, or tingling in your foot, ankle, or lower leg may develop
- Weakness or rapid fatigue
- The muscles of your leg may feel weak
- Muscles may feel tired or may become more rapidly fatigued than normal
- Pain or pressure at the affected site
- A feeling of pain or pressure may exist in the region of a deep vein thrombosis
- The most common example is a thrombosis formation in the calf, and pressure on your calf muscle will be painful
A medical emergency: symptoms of a pulmonary embolism
If you experience the following symptoms, call 9-1-1 or seek immediate medical attention as this may be a life threatening situation:
- Sudden shortness of breath without exertion
- Increased heart rate without exertion
- Pain in the chest, particularly with deeper breaths or coughing
- Dizziness, feeling light-headed, or fainting
- Coughing up blood

Common mechanism of deep vein thrombosis
For gamers, deep vein thrombosis will most likely occur due to prolonged sitting and lack of physical activity—specifically, a lack of weight-bearing activity that requires contraction of the calf and thigh muscles.
This mechanism is specific to gamers absent of blood clotting disorders or other pre-existing cardiovascular conditions. It is important to schedule an annual physical (wellness check-up) with your doctor to screen for these types of pre-existing conditions.
Prevention
Absent of pre-existing blood or cardiovascular disorders, the most common mechanism of deep vein thrombosis is physical inactivity.
Therefore, prevention is quite simple—physical activity; performing simple movements routinely during gaming sessions and exercising regularly will significantly reduce your risk.
Additionally, lifestyle factors that decrease the risk for deep vein thrombosis include eating a healthy diet (read our post on the basics of nutrition) and not smoking cigarettes.
Mid-session movements to prevent deep vein thrombosis
- Seated calf raises and toe raises (every 15-20 minutes)
- Press up on your toes so your heels are elevated off the ground
- Then, return your heels down and lift your forefoot off the ground
- Repeat this alternating pattern 10 times total
- Standing calf raises (every 30-60 minutes)
- Perform 5-10 standing calf raises with both legs
- You do not need to add resistance; simply perform 5-10 calf raises with your body weight
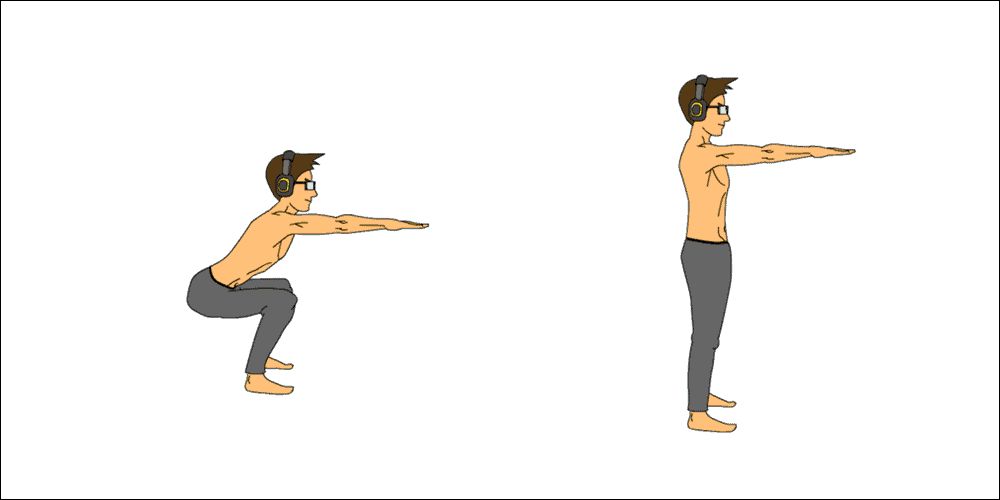
- Squats or lunges (every 30-60 minutes)
- Perform 5-10 squats or 5-10 lunges (on each leg)
- Again, you do not need to add resistance; simply perform 5-10 squats or lunges with your body weight
Treatment
If you are experiencing the symptoms listed above, a deep vein thrombosis can be confirmed with an ultrasound. Most often, this will be the first screening test due to its accuracy, safety, ease of use, and cost-effectiveness. Once confirmed, you should speak with your doctor about treatment options.
References
- Tovey C, Wyatt S. Diagnosis, investigation, and management of deep vein thrombosis. BMJ. 2003; 326:1180-4.
- Kesieme E, Kesieme C, Jebbin N, Irekpita E, Dongo A. Deep vein thrombosis: A clinical review. Journal of Blood Medicine. 2011; 2:59-61.
- Scarvelis D, Wells P. Diagnosis and treatment of deep-vein thrombosis. CMAJ. 2006; 175(9):1087-92.
- Stubbs MJ, Mouyis M, Thomas M. Deep vein thrombosis. BMJ. 2018; 360:k351.
