Sciatica in gamers: an undeniable pain in the butt
Key points
Disclaimer
This information is for educational purposes only and is not intended to replace the advice of your doctor. Esports Healthcare disclaims any liability for the decisions you make based on this information.
The information contained on this website does not establish, nor does it imply, doctor-patient relationship. Esports Healthcare does not offer this information for diagnostic purposes. A diagnosis must not be assumed based on the information provided.
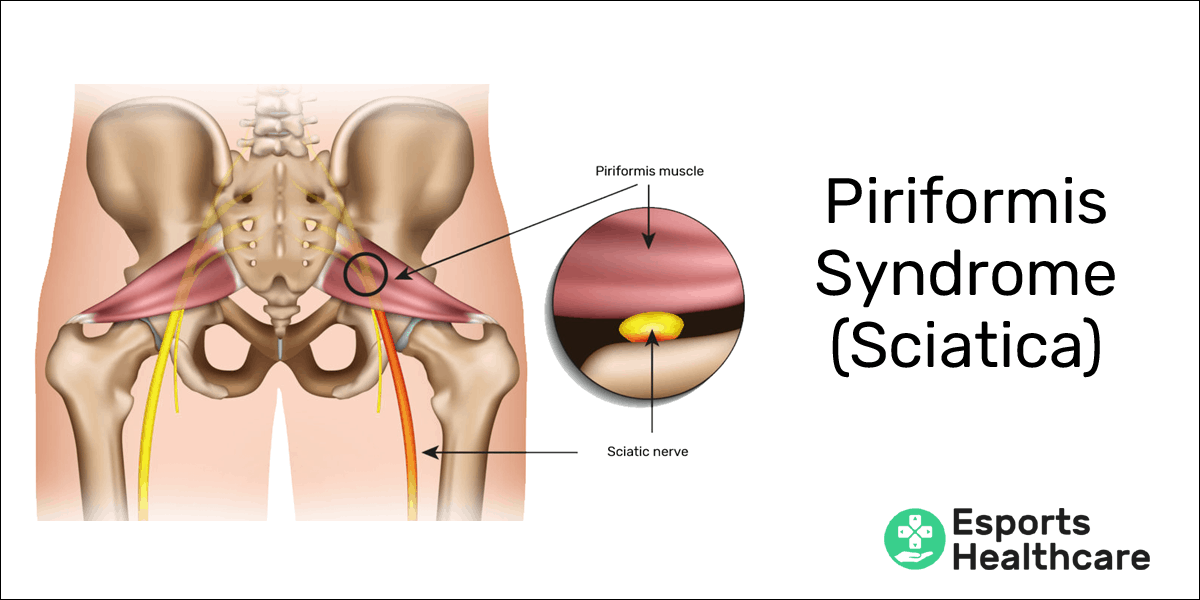
What is sciatica (piriformis syndrome)?
Sciatica is the name for pain patterns caused by direct irritation of the sciatic nerve—most notably in the back of the thigh and leg. The sciatic nerve is most often irritated by the piriformis muscle, a hip muscle that exits the pelvis through the same opening as the sciatic nerve.
For gamers, sciatica usually occurs due to prolonged sitting and is exacerbated by poor posture. Refer to our guide for gamer posture to reduce your risk for the piriformis muscle causing sciatica.
Another condition that causes sciatic-type symptoms is spinal nerve root impingement. This condition is also known as lumbar radiculopathy and can present with pain patterns mirroring sciatica. However, true sciatica is direct impingement of the sciatic nerve in the gluteal region, and this page will focus on this condition.
Pertinent anatomy
It’s important to know some basic anatomy of the lumbar spine and pelvis to understand sciatica.
To begin, the sciatic nerve is the largest nerve in the human body. It is a collection of lumbar and sacral nerve roots that provides motor control for large portions of the thigh, leg, and foot. Through its terminal branches, the sciatic nerve also supplies touch sensation for the lower leg and foot.
For each bone in your spine, there is an associated nerve root that corresponds with an area of the body. In the lower back, nerve roots L4, L5, S1, S2, and S3* combine to form the sciatic nerve.
* Nerve roots are the first nerve branches off the spinal cord. The letters and numbers refer to the spinal region and segment. The letter “L” refers to the lumbar spine and “S” refers to the sacrum. There are 5 lumbar bones and nerve roots, and the sacrum bone has 4 of its own nerve roots.
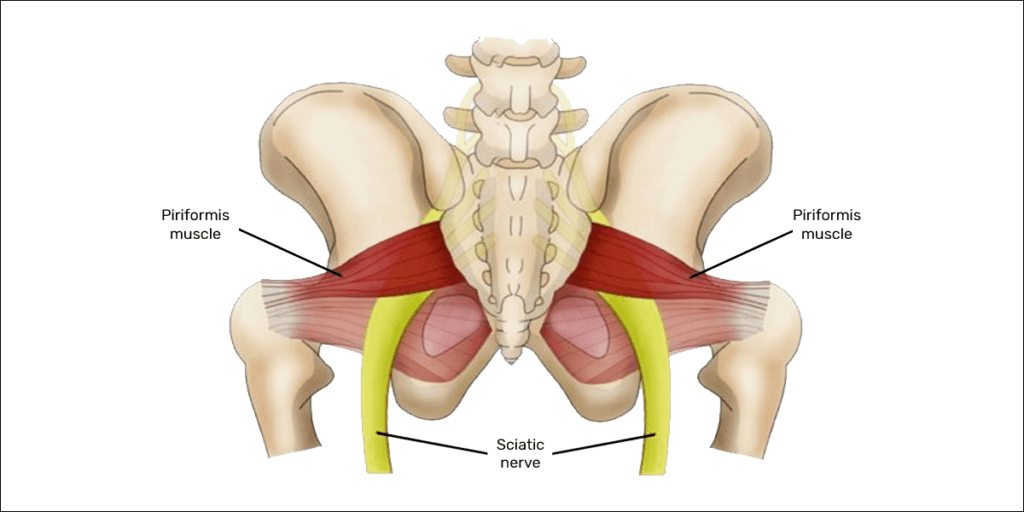
Sciatic nerve
Nerve roots L4 through S3 combine to form the sciatic nerve within the pelvis. The sciatic nerve then exits into the gluteal region through an opening in the pelvis called the greater sciatic notch. Through this same notch, the piriformis muscle also exits the pelvis to attach to the femur (thigh bone).
In the thigh, innervation of the sciatic nerve is motor only; it does not include cutaneous (skin sensation) innervation. The muscles of the sciatic nerve are the hip external rotator muscles and the muscles in the posterior compartment of the thigh:
- Hip external rotator muscles: these muscles all turn the thighs outward
- Gemellus superior
- Gemellus inferior
- Obturator internus
- Obturator externus
- Posterior thigh compartment muscles (the hamstring group): these muscles extend the hips and flex the knees
- Semitendinosus
- Semimembranosus
- Biceps femoris
Just above the knee, the sciatic nerve splits into 2 branches: the common peroneal nerve and the tibial nerve. These nerve branches innervate the muscles in the lower leg, ankle, and foot. These nerve branches also include cutaneous innervation to the lower leg and foot with the exception of the medial (inner) portion.
Pathophysiology
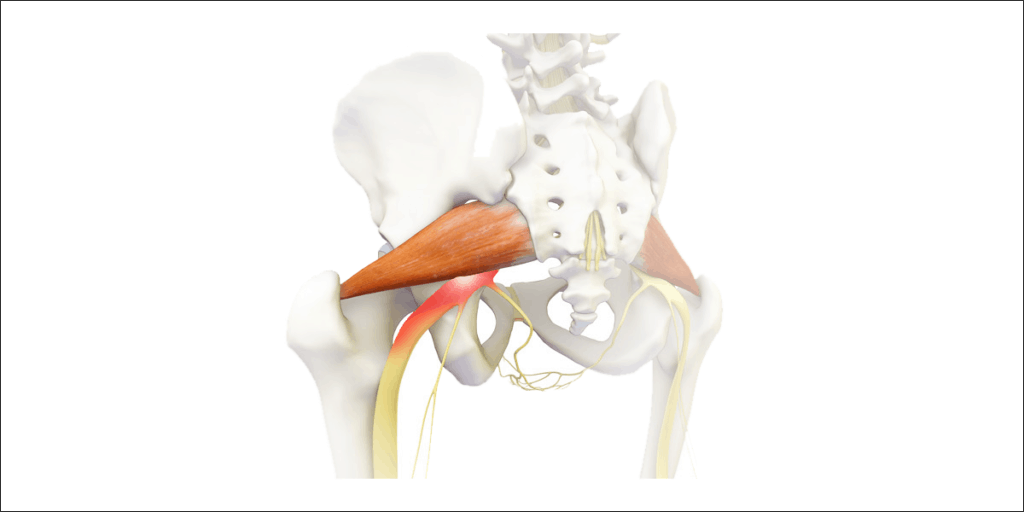
Sciatica occurs when there is compression or irritation of the sciatic nerve. The compression or irritation may be caused by:
- Piriformis syndrome
- This is the most common cause. Tightness or spasm in the piriformis muscle impinges the sciatic nerve directly where both structures exit through the pelvis through the greater sciatic notch
- Direct compression of the sciatic nerve
- Prolonged or awkward seated posture: sitting awkwardly or for long periods of time can compress the sciatic nerve, directly
- Lumbar nerve root impingement
- Impingement or irritation of any individual lumbar nerve root, L4 through S3, may cause sciatic-type symptoms; however, this is not a true sciatica
- Lumbar nerve root impingement may occur from lumbar disc herniation or other stenosis (narrowing) of the neural canal
Signs and symptoms
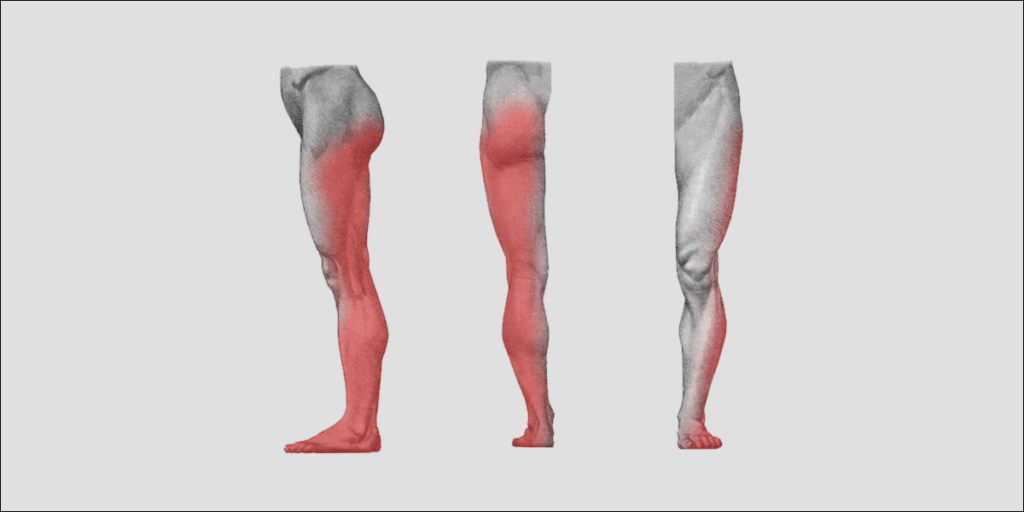
Since the sciatic nerve contains nerve roots L4 through S3, the possible affected area is quite large:
- The back or outer portion of your thigh
- The nerve itself may feel painful in this region, but the skin will not have altered sensation
- The back, front, or outer portion of your lower leg (nerve and skin sensation)
- The majority of the skin of your foot excluding a small area on the inner portion (nerve and skin sensation)
In these regions, sciatica will present as one or more of the following symptoms:
- Numbness and tingling
- Many times, the first sign is a change in sensation which may include pins and needles, numbness, and/or tingling
- Pain
- Sciatic-type pain is often described as sharp-shooting or burning
- Weakness
- You may experience difficulty in flexing your knee or performing any action of your ankle joint
Sciatica will not present as pain, numbness, tingling, or weakness in the inner portion of the thigh, lower leg, or foot. These symptoms are instead associated with femoral nerve impingement or nerve root irritation T12 through L3.
Note: if you experience the above-listed symptoms along with swelling of the leg, ankle, or foot, paleness or blue color, and/or cool or cold sensation, these are signs of a more serious condition. You should consult your doctor or visit the emergency room if you experience these symptoms.
Common mechanism(s) of injury

Sciatica is more likely to occur in people who sit for prolonged periods of time, especially if the seated posture is awkward or off balance. Prolonged sitting or awkward position may cause irritation in two ways:
- Direct compression
- Constant pressure on the gluteal region and back of the thighs may compress the sciatic nerve, directly
- A well-cushioned chair will make it less likely for sciatic nerve compression to occur
- Chronic muscle tightness in the piriformis or hamstrings
- Sitting for extended periods of time may lead to hypertonicity (tightness) which can cause crowding or compression of the sciatic nerve
- Sitting awkwardly (e.g., legs crossed or feet not flat on the floor) may put unnecessary tension on muscles leading to strain and tightness
Prevention
The most common mechanisms of injury for sciatica are direct compression of the sciatic nerve and poor and/or prolonged static position.
- Body position: check out our posture education page to check your seated posture and reduce the risk of developing sciatica.
- Sit with your hips all the way back in the chair so your back is pressed against the backrest
- Keep both thighs flat on the chair
- The chair height should allow your feet to rest flat on the floor with no additional strain on your legs
- Your knees should be bent approximately 90 degrees
- Rest both feet flat on the floor below your knees
Take breaks: for every half hour you’re sitting, you should stand up and walk around for 5 minutes!
Rehabilitation
To effectively resolve sciatica, it is important to first identify and correct the initial cause. For example, if you’re sitting too frequently without taking breaks or if you’re sitting awkwardly, protocols may be ineffective because of the constant exacerbation.
In practice, the following treatments are effective for the treatment of piriformis syndrome:
- Manual therapy techniques (e.g., pressure release) of the piriformis muscle
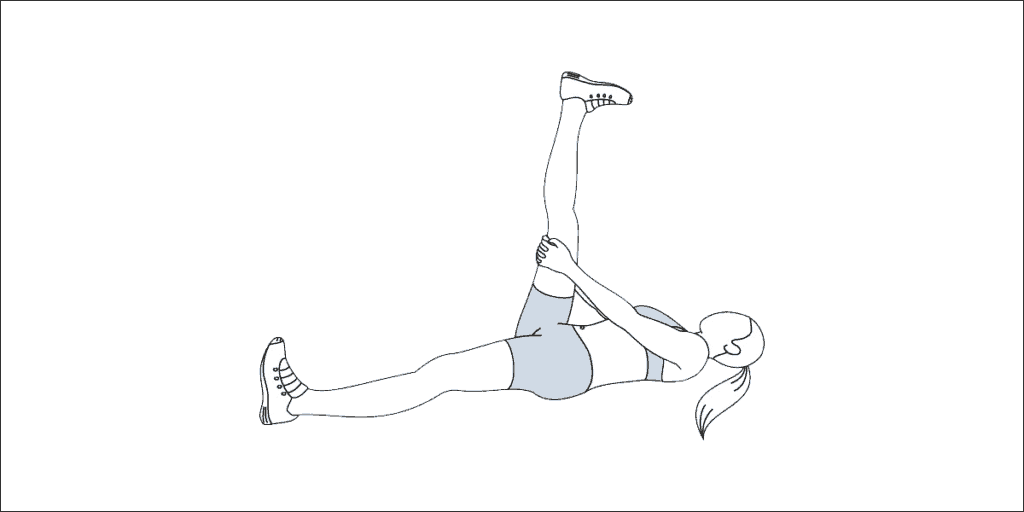
- Post-isometric relaxation stretch of the piriformis muscle
- Post-facilitation stretch of the hamstrings
- Heat therapy in the gluteal region
- Therapeutic exercises
- Functional Range Conditioning (FRC®): 90/90 hip PAILs/RAILs
- Hip mobility exercises (FRC®: hip CARs)
- Sciatic nerve glide
- Education in proper ergonomics
Hypervolt+ percussion massage

Esports Healthcare will also utilize the Hypervolt+® percussion tool for treatment of piriformis syndrome.
To your tolerance, the Hypervolt+® can be used to massage the the piriformis muscle in the gluteal region. Please note, this treatment may be painful to endure.
